Is It Schizophrenia? Is It Substance Use?
Around ten million adults in the United States currently experience both mental illness and a substance use disorder (SUD). It’s a well-established correlation, often complicating the treatment of both conditions. One such co-occurring disorder is schizophrenia
In a recent webinar for Harmony Foundation, Colorado Recovery’s medical director Alan Fine, M.D., talked about the symptoms of schizophrenia and substance use disorder and why it is frequently difficult to tell the two conditions apart.
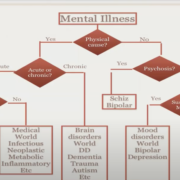
First off, Dr. Fine presented a diagnostic flowchart to illustrate where SUD and schizophrenia can be found in the mental healthcare realm. If the symptoms are acute and were caused by taking drugs or drinking alcohol then we’re looking at substance misuse and a possible addiction scenario. If the diagnosis is psychosis without a physical cause, the condition is often diagnosed as schizophrenia or bipolar disorder.
The diagnosis of schizophrenia itself is complicated and based on the work of three trailblazers in the field whose impact can still be felt today: Emil Kraepelin (1856–1926), Eugen Bleuler (1857–1939), and Kurt Schneider (1887–1967).
Kraepelin is considered one of the founders of modern scientific psychiatry. His views dominated the field at the start of the 20th century. Bleuler renamed Kraepelin’s “dementia praecox” schizophrenia and established the classic four As of the condition: ambivalence, affect, alogia, and autism (preoccupation with self). Schneider in turn formulated the first-rank symptoms of schizophrenia: auditory hallucinations, feelings of external control, thoughts connected to others, and other delusions.
In his book, The Environment of Schizophrenia, Colorado Recovery founder Richard Warner wrote that “schizophrenia is a psychosis. That is to say, it is a severe mental disorder in which the person’s emotions, thinking, judgment, and grasp of reality are so disturbed that his or her functioning is seriously impaired.”
What about substance use then?
By definition, schizophrenia is not caused by the effects of a substance or another medical condition. That, however, is not quite all.
Mental health conditions and SUDs frequently co-occur because many people with addiction are primarily misusing addictive substances to self-medicate emotional pain caused by serious mental health disorders.
“The proportion of schizophrenic patients of comorbidity of substance abuse varies in published studies from 10–70 percent, depending on how patients are diagnosed with schizophrenia, the types of populations studied, and the different ways of defining drug and alcohol disorders,” said Dr. Fine. “There’s a remarkable overlap in both directions.”
People with schizophrenia are at a higher risk of engaging in substance misuse because many of them will be tempted to self-medicate the severe symptoms of their mental illness as well as some of the side effects of their antipsychotic medications. At the same time, substance misuse may cause syndromes that are similar or even identical to schizophrenia.
In the short term (acute intoxication), schizophrenia-like symptoms may include delusions (stimulants and inhalants), loose associations (stimulants, alcohol, sedatives, and inhalants), and hallucinations (stimulants, alcohol, and inhalants). Both alcohol and sedative withdrawal symptoms include hallucinations and paranoia.
In the long term (prolonged misuse), “amphetamine use is associated with long-term psychosis—thirty percent of all amphetamine-induced psychoses become chronic,” Dr. Fine explained. Chronic alcohol misuse may cause persistent dementias such as Korsakoff syndrome and delirium tremens.
People with schizophrenia also engage in substance misuse to cope with the deterioration of their social environment, an area that Dr. Warner explored extensively.
So, the answer to the question “Is It schizophrenia or is it substance misuse?” is often: both! That means, should both conditions be present, both need to be treated because they may reinforce each other. An important element in this regard is empowerment.
Empowering people with schizophrenia reduces the need to self-medicate and often improves symptoms. Believing in their ability to take charge of their lives and manage the complex challenges of their illness is crucial for people with schizophrenia.
Over the course of his long professional career, the late Dr. Warner realized that social inclusion empowers people with mental illnesses and improves outcomes. “Work helps people recover from schizophrenia,” Warner concluded. “Productive activity is basic to a person’s sense of identity and worth.”
Colorado Recovery has been utilizing the Warner method to empower adults with mental illness for many years now. Our treatment facility provides the services needed to address schizophrenia, bipolar disorder, and other serious mental illnesses. Call us at 720-218-4068 to discuss treatment options for you or the person you would like to help.